Comments (2)
Karen Robson
Healthcare is weak in the United States
Alex Barber
Good analysis as always

When it comes to maternal mortality during pregnancy, the United States not only lags behind other high-income countries, but has been getting worse.
The National Academies of Sciences, Engineering, and Medicine tells the story in its report Birth Settings in America: Outcomes, Quality, Access, and Choice. Here's the trendline of US maternal mortality over time:
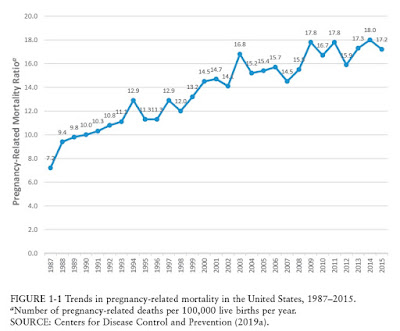
As part of putting this in (grim) perspective, the report notes (citations omitted):
In contrast, the rate of maternal mortality has consistently dropped in most high-resource countries over the past 25 years. Severe maternal morbidity has been increasing in the United States as well. It is estimated that for every woman who dies in childbirth, 70 more come close to dying . All told, more than 50,000 U.S. women each year suffer severe maternal morbidity or “near miss” mortality, and roughly 700 die, leaving partners and families to raise children while coping with a devastating loss. Like the rates of maternal mortality, U.S. rates of severe maternal morbidity are high relative to those in other high-resource countries. In this context, it is notable that some local efforts in the United States have shown progress in reducing rates of maternal mortality and morbidity. In California, for example, the California Maternal Quality Care Collaborative led an initiative that reduced rates of maternal mortality by 55 percent (from 2006 and 2013) ...
The fundamental problem here doesn't seem to be an issue of too little overall spending, but more of misallocated spending. US overall healthcare spending is high, and costs of childbirth are a big part of that. The NAS report notes (citations omitted):
Childbirth is the most common reason U.S. women are hospitalized, and one of every four persons discharged from U.S. hospitals is either a childbearing woman or a newborn . As a result, childbirth is the single largest category of hospital-based expenditures for public payers in the country, and among the highest investments by large employers in the well-being of their employees. Cumulatively, this spending accounts for 0.6 percent of the nation’s entire gross domestic product, roughly one-half of which is paid for by state Medicaid programs.
The discussion in the report suggests that there is too little spent on prenatal care, perhaps some overview of (costly) hospitals as a venue for births compared with other options, and an overuse of some costly care like C-sections.
A natural concern is how this might relate to infant mortality. However, US infant mortality has been falling over time. The two main concerns in this area seem to be a rise in the share of children born with low birthweights, together with large discrepancies across groups. Here's a figure on low birthweights from a National Center for Health Statistics Data Brief in 2018:
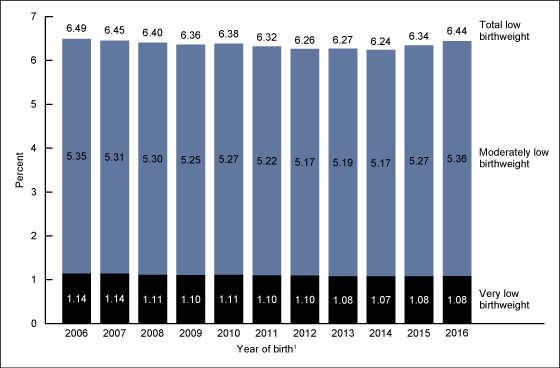
Here's the NAS report on infant mortality differences across groups (citations and references to figures omitted).
In contrast to maternal mortality, infant mortality in the United States has been declining over the past 20 years, and there are expanded opportunities for survival at increasing levels of prematurity and illness complexity. However, large disparities persist among racial/ethnic groups and between rural and urban populations. In 2017, infant mortality rates per 1,000 live births by race and ethnicity were as follows: non-Hispanic Black, 10.97 per 1,000; American Indian/Alaska Native, 9.21 per 1,000; Native Hawaiian or Other Pacific Islander, 7.64 per 1,000; Hispanic, 5.1 per 1,000; non-Hispanic White, 4.67 per 1,000; and Asian, 3.78 per 1,000. ... Rates of preterm birth and low birthweight have increased since 2014, and as with other outcomes, show large disparities by race and ethnicity. Low-birthweight (less than 5.5 pounds at birth) and preterm babies are more at risk for many short and long-term health problems, such as infections, delayed motor and social development, and learning disabilities. About one-third of infant deaths in the United States are related to preterm birth ...
The NAS report does not offer a lot of clear recommendations for what should be done. The discussion of steps that could be taken for quality improvement (QI) is full of statements like: "While many QI initiatives have shown promising results, many current QI initiatives are underfunded." Do tell. But the report does offer some possible models to follow, like the California Maternal Quality Care Collaborative mentioned earlier.
A version of this article first appeared on Conversable Economist.
Healthcare is weak in the United States
Good analysis as always
Timothy Taylor is an American economist. He is managing editor of the Journal of Economic Perspectives, a quarterly academic journal produced at Macalester College and published by the American Economic Association. Taylor received his Bachelor of Arts degree from Haverford College and a master's degree in economics from Stanford University. At Stanford, he was winner of the award for excellent teaching in a large class (more than 30 students) given by the Associated Students of Stanford University. At Minnesota, he was named a Distinguished Lecturer by the Department of Economics and voted Teacher of the Year by the master's degree students at the Hubert H. Humphrey Institute of Public Affairs. Taylor has been a guest speaker for groups of teachers of high school economics, visiting diplomats from eastern Europe, talk-radio shows, and community groups. From 1989 to 1997, Professor Taylor wrote an economics opinion column for the San Jose Mercury-News. He has published multiple lectures on economics through The Teaching Company. With Rudolph Penner and Isabel Sawhill, he is co-author of Updating America's Social Contract (2000), whose first chapter provided an early radical centrist perspective, "An Agenda for the Radical Middle". Taylor is also the author of The Instant Economist: Everything You Need to Know About How the Economy Works, published by the Penguin Group in 2012. The fourth edition of Taylor's Principles of Economics textbook was published by Textbook Media in 2017.
Leave your comments
Post comment as a guest