Comments (3)
Daniel Ribeiro
Very helpful! Did not know some of this - thanks for the information
Kumar Mohit
Another great article
Willam Paterson
Enlightening post
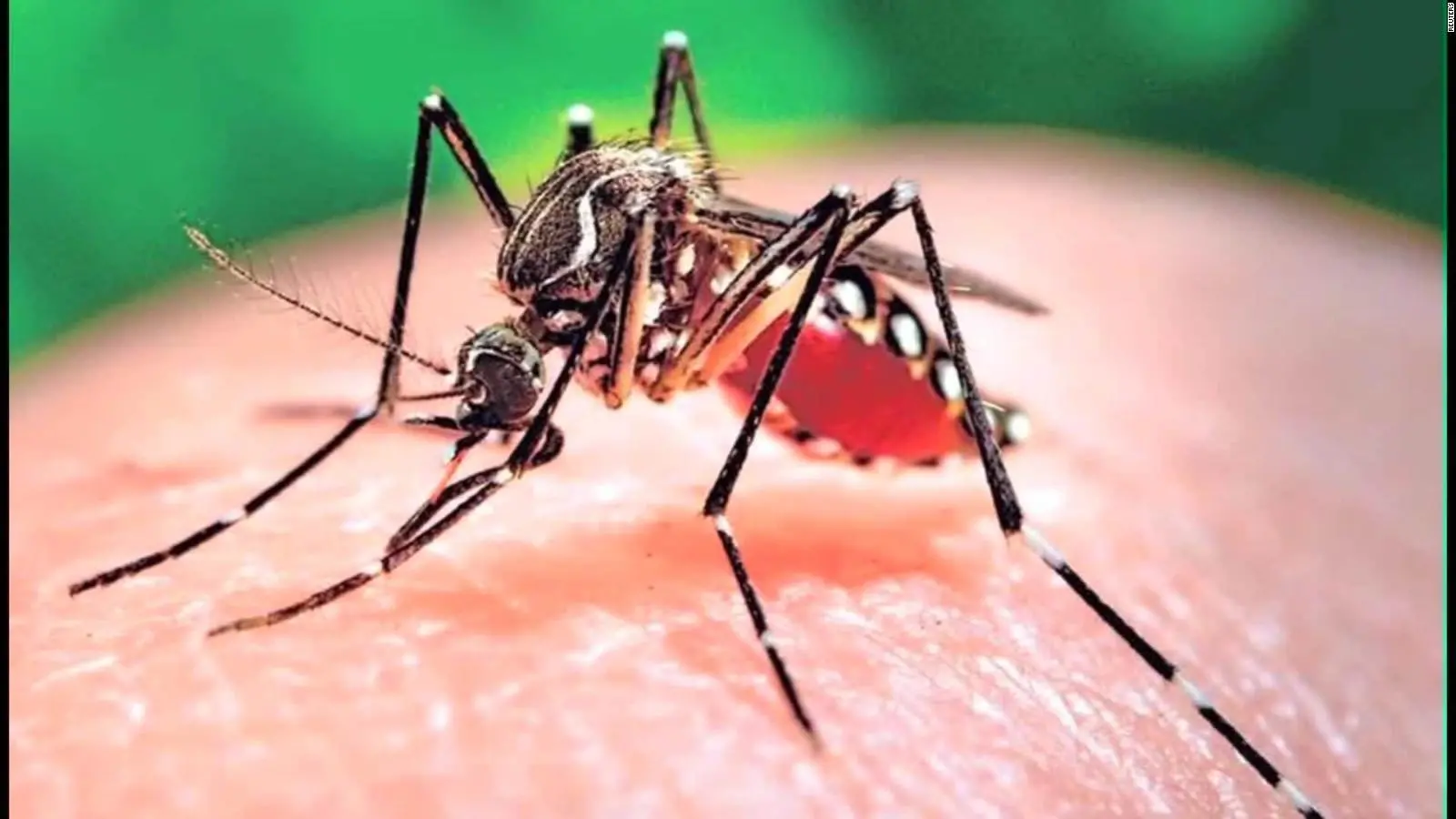
The CDC issued a report this past week highlighting dramatic increases in the rates of infectious diseases spread by ticks, fleas, and mosquitoes- otherwise known as “vector-borne diseases.” That list includes some long-familiar scourges, such as Lyme disease; some rather new to our lexicon in this part of the world, like Zika; some seemingly resurrected from Medieval parchment, like plague; and some long considered someone else’s problem, like dengue.
Covered by all of the major news outlets, the report is as important for what it barely says, as for what it asserts explicitly and emphatically. What’s emphatic is that rates of vector-borne disease have more than tripled in the U.S. in the past decade alone. That toll involves both more of the diseases we had reason to dread all along, such as Lyme, and threats formerly all but unknown here- such as the tropical disease, Chikungunya. What is explicit is that our public health and environmental systems are ill-prepared to contain this threat. Our resources are inadequate across the spectrum of treatment, surveillance, prevention, and control of the vector populations.
But what matters most is almost certainly what the report barely says, or omits entirely, about the reasons for this. Emerging infections are the result of changes in exposure, and those in turn result when people and pathogens find themselves together in new places, or when the environmental conditions of previously populated places change, making them hospitable to new agents of disease.
Both of these phenomena are occurring, in the U.S. and globally. The single greatest manifestation of environmental change is the climate. Media coverage of the CDC report all note in a seemingly understated way how understated the references to climate change are in the report. It is, as ever, the inconvenient truth.
I live in Connecticut, where after the coldest, wettest, least spring-like spring in memory, we transitioned immediately to temperatures in the mid 90s in early May- weather that would constitute a heat wave in mid-August. That’s unsettling for us humans, but ticks never seem to mind.
I have three dogs, and a horse. I hike and ride through the New England woods every chance I get. The result is that I am among those vulnerable to getting vector-borne diseases; tick check is a routine operation here. I have treated myself for early Lyme twice. We have treated at least two of our dogs for Lyme as well, and my horse- also twice. On one occasion, I acquired another tick-borne disease, anaplasmosis, that resulted in an ER visit, a CT of my head, a spinal tap, and then hospital admission. At the peak of it, I felt like I might die, and to be honest, was rather hoping I would just to end the excruciating, total body pain. I am glad to report I recovered fully. I would really rather not do it again. Nor am I the only member of my immediate family to suffer vector-borne torments.
I mention all this to make it clear that the dangers are not just clear and omnipresent, but up close and personal, too. I have very literal skin in the game, and as much reason to be worried about increasing vector-borne diseases as anyone else. But it is our failure to address root causes that worries me far more.
We have an exact analogy in chronic diseases, such as heart disease, diabetes, cancer, and dementia. In this area, we received a provocative memo 25 years ago regarding underlying, “root” causes, and the critical need to address them. We have largely ignored that memo, and the result is that despite amazing advances in treatment, we have a massive increase in the burden of chronic disease, not the decrease that has long been achievable.
Among the root causes of emerging and surging vector-borne diseases is a changing climate, for which we are obviously responsible. We cannot hope to manage the effect when systematically neglecting the cause.
The other factor- people and pathogens coming together in new places- is also a salient contributor, to some extent in the U.S., where our current environmental policies favor development over conservation - and even more so around the world. Globally, environmental encroachment is less a matter of presumption, privilege, and greed as it is here, and more a matter of basic human need. People move into new environments because there are too many people in familiar ones; because there isn’t enough land, or food, or water. The global population is a major driver of this, as is a failure to manage natural resources in ways that strike sustainable balances.
There are ways to address such things. There are shining examples of how to empower people with the means to produce their own food in sustainable ways; efforts to conjoin the health of people and planet; brilliant innovations that turn environmental conservation, clinical care, and economic opportunity into a single, harmonious continuum.
But these are exceptions rather than rules, and never more so than now when the EPA seems to conspire actively against the environment, and when inconvenient scientific realities are simply declared inadmissible, and expunged from the policy dialogue. But while we may choose not to talk about what we wish weren’t true, we may be certain the ticks, and fleas, and mosquitoes don’t give a damn.
Public health and prevention seem only ever to get the love and resources they warrant in the fleeting aftermath of the latest calamity. We are presumptuous and arrogant enough never to mind our place in a nature greater than ourselves. We are greedy and shortsighted enough to feign acute concern with effects, while systematically neglecting causes of our own devising.
Nature’s minions- ticks, and fleas, and mosquitoes- don’t ever mind. They just adapt to exact an inevitable toll.
Stated differently, at times the only reliable defense of the human body derives from an enlightened body politic. While waiting, good luck out there.
Very helpful! Did not know some of this - thanks for the information
Another great article
Enlightening post
David L. Katz, MD, MPH, FACPM, FACP, FACLM, is the Founding Director (1998) of Yale University’s Yale-Griffin Prevention Research Center, and former President of the American College of Lifestyle Medicine. He has published roughly 200 scientific articles and textbook chapters, and 15 books to date, including multiple editions of leading textbooks in both preventive medicine, and nutrition. He has made important contributions in the areas of lifestyle interventions for health promotion; nutrient profiling; behavior modification; holistic care; and evidence-based medicine. David earned his BA degree from Dartmouth College (1984); his MD from the Albert Einstein College of Medicine (1988); and his MPH from the Yale University School of Public Health (1993). He completed sequential residency training in Internal Medicine, and Preventive Medicine/Public Health. He is a two-time diplomate of the American Board of Internal Medicine, and a board-certified specialist in Preventive Medicine/Public Health. He has received two Honorary Doctorates.
Leave your comments
Post comment as a guest