The "curse of knowledge" refers to a well-known behavioral bias: when you know something, it's hard to remember what is was like not to know it.
One standard example is a teacher who knows the subject extremely well, but fails to communicate with students because the teacher can no longer remember what it was like not to know the subject. At this point, we all know that the COVID-19 pandemic has caused more than 200,000 deaths in the United States alone. Along with the health costs, we have experienced the businesses closing, the lockdowns affecting schools and churches, and the many disruptions of everyday life. It's hard to avoid our own "curse of knowledge," and think back to those long-age moments of February and early March 2020 when at least most of us didn't know what to make of the pandemic.
In the Fall 2020 issue of the Journal of Economic Perspectives, we have a two-paper Symposium on Economics and Epidemiology--one paper by a group of economists aimed introducing basic epidemiology of infectious diseases, and the other by an epidemiologist looking back from the perspective of that field. Today and for the next couple of days, I'll draw on these articles to take a look back at what what we were thinking before we knew what we know now. Some lessons for when (not if) the next pandemic arrives will naturally suggest themselves. The two JEP papers are:
- "An Economist's Guide to Epidemiology Models of Infectious Disease," by Christopher Avery, William Bossert, Adam Clark, Glenn Ellison and Sara Fisher Ellison (pp. 79-104)
- "Epidemiology's Time of Need: COVID-19 Calls for Epidemic-Related Economics," by Eleanor J. Murray (pp. 105-20)
As the Avery et al group point out at the start of their paper, there was a strong shift in attitudes about the COVID-19 pandemic in mid-March 2020. In the US, for example, they note:
"[O]n March 11, President Donald Trump reassured the American people that for “[t]he vast majority of Americans, the risk is very, very low.” Just five days later, the Trump administration recommended that “all Americans, including the young and healthy, work to engage in schooling from home when possible. Avoid gathering in groups of more than 10 people. Avoid discretionary travel. And avoid eating and drinking at bars, restaurants, and public food courts” ...
A similar shift happened in the United Kingdom. What changes? On March 16, a prominent group of epidemiologists at Imperial College in London published a study with estimates that the death toll of the pandemic could reach 2.2 million in the United States and 500,000 in the United Kingdom. The specific study was "Report 9: Impact of non-pharmaceutical interventions (NPIs) to reduce COVID-19 mortality and healthcare demand," written by Neil M Ferguson and a long list of co-authors "on behalf of the Imperial College COVID-19 Response Team." The first figure in the report looked like this:
The report also placed a heavy emphasis on how hospitals and health care providers could be overwhelmed by this projected death toll. The report is very clear in noting that this prediction is based on the absence of any policy or individual changes:
In the (unlikely) absence of any control measures or spontaneous changes in individual behaviour, we would expect a peak in mortality (daily deaths) to occur after approximately 3 months (Figure 1A). In such scenarios ... we predict 81% of the GB and US populations would be infected over the course of the epidemic.
This particular forecast took on particular force. It was often criticized for being a naive estimate, because it assumed no public or individual response. The deeper meaning is that those who made this criticism had not apparently looked at the report. Most of the report is a discussion of strategies for suppression or mitigation of the virus, with a detailed look at the possible effects of "non-pharmaceutical interventions" including case isolation, voluntary quarantine, social distancing of those 70 and older, social distancing of the entire population, and closure of schools and universities. There are charts showing the effects of different combinations of these strategies: for example, one chart suggests that with these kinds of measures in place, the overall death toll could be reduced 50-fold, from over 500,000 in the UK to less than 10,000, with similar estimates for the US.
In short, the Imperial College study from back in March 2020 was often dramatically mischaracterized. Yes, their model suggests 2.2 million US deaths and 510,000 UK deaths is in the report if there was zero response by the public sector or by individuals. But the report was not expecting or predicting a response of zero! Instead, the report was trying to show how a variety of interventions could affect the death toll. To put it another way, the report was trying to show the dangers of inaction and the benefits of action.
But there's a powerful irony here. Although many commenters were quick to note that the top of the bell-shaped curve of the figure above was based on a lack of public or private response, many of the same commenters seemed to accept the overall shape of the bell-shaped curve--and its implicit prediction that the novel coronavirus would pass through the population and be done in a few months. say by early July. For example, knowledgeable observers like former Fed chairman Ben Bernanke were saying in late March that the pandemic was like a giant snowstorm--something that would dramatically slow economic activity for a time but then would pass.
The emphasis back in March 2020 was that having everyone stay at home as much as possible for a couple of weeks would buy time so the health care system wouldn't be overloaded. The original relief bills passed by Congress envisioned financial support for workers and firms that would only need to last for a couple of months. For example, back in March 2020, pretty much no one was talking about how we might still be talking about keeping all K-12 schools, colleges and universities, or churches closed by late 2020. We weren't talking about waves of COVID-19 that could last for a year or more.
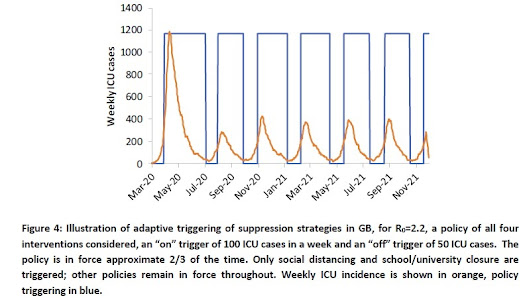
The Imperial College report back in March 2020 actually spelled out this kind of scenario. For example, it considered what would happen if the non-pharmaceutical interventions to mitigate the pandemic would be switched on and off over time, depending on the capacity of the health care system. The idea was that when infections surged, then the mitigation measures would be tightened, and at other times they would be eased back. The resulting simulation was that the pandemic would come in a series of waves over time, as the March 2020 report showed in figures like this one:
Notice that in this "adaptive triggering of suppression strategies," the pandemic is having a wave about every three months through 2021.
In taking a deeper look into the epidemiology models, the Avery et al. team note that this assumption of a bell-shaped curve of infections has been standard for a long time--but it's a pattern that applies for epidemics that are not effectively controlled. In addition, Murray points out in her essay that the problem at the beginning of any epidemic is that the data is very limited and the characteristics of the disease (methods of transmission, health effects, and so on) are never fully known. She writes:
But to put these concerns in real-world context, no infectious disease modeler expects to be able to accurately forecast the future based on sparse data from early in a pandemic. Even “nowcasting,” the task of modeling the current number of true infections, is extremely challenging, especially early in a pandemic. Asking an infectious disease modeler to predict the exact trajectory of an outbreak is akin to asking an economist to select stocks for your portfolio or a climate scientist to predict the best day in 2022 for an outdoor wedding. These tasks, while of interest to many people, are not generally within the purview of scientists. Instead, the goal of both mechanistic and phenomenological models in epidemiology is to forecast a range of possible futures, given a specified set of assumptions. ...
In the case of the Imperial College model, two of the key assumptions which defined their original model were that the government would not respond to the COVID-19 pandemic with any interventions and that the general public would not respond to the pandemic with any changes to their own behavior. These assumptions are clearly unrealistic. However, by making these strong assumptions, the Imperial College model was able to provide epidemiologists and public health practitioners with a rapid estimate of the worst-case scenario: if SARS-CoV-2 was allowed to run unchecked through the population, what is the maximum amount of death that we might expect over the course of the outbreak until it burned out via herd immunity? The answer––510,000 deaths in the United Kingdom and 2,200,000 in the United States (Walker et al. 2020)—rightly spurred both governments and individuals to action.
What lessons does this experience hold for the next pandemic? One obvious lesson is to go beyond the big death estimate in the headlines (2.2 million will die!) or the simple criticism on social media (the estimate ignores public and private actions!) and look at the actual underlying report and arguments. At a deeper level, there seems to be a tradeoff to face: a country can have a uncontrolled pandemic with high health costs that passes through the population fairly quickly and is finished, or it can have a semi-controlled pandemic with a lower death rate that lasts for a much longer period. Be wary if you see a bell-shaped prediction of how a pandemic will shoot high and then fall to zero, and remember that this pattern really only holds if the pandemic is uncontrolled.
Public health authorities should be very hesitant before making statements that seem to imply that a pandemic will be over fairly soon. If actions are taken and the pandemic is not over soon, people will remember the earlier statements and the public health authorities will lose some credibility that their recommendations are useful at all. Yes, it would have been a lot harder back in March 2020 to say that the short-term shutdown was really just to avoid a catastrophic outcome and reduce the death toll, but that the pandemic was likely to go on for months and additional shutdowns would probably be needed over time. But that explanation would have been an honest reading of the March 2020 Imperial College report.
Similarly, public policy actions to help workers and firms at the start of the pandemic shouldn't be based on an implicit assumption that the pandemic will be a short-term event. By all means, act quickly to offer some short-term assistance. But bear in mind that you are need to think about what will be sustainable for perhaps a year or more into the future, not just the next few months.
A final lesson is that while financial support for those affected by a pandemic and various non-pharmaceutical interventions all have their place, government may also have an important role to play in facilitating and smoothing transition. It's of course hard to know how the actions of people, firms, and other institutions might have changed with different advice and policy. But one can at least imagine a situation where national groups were convened back in April to start thinking about best-practice recommendations for workplaces, schools and universities, health care, retail, restaurants, theaters, and other sectors of the economy. Perhaps a vision could have developed of the kinds of adjustments that might be sustainable over time in these various environments, along with investments like making sure more people (adults and children) had reliable at-home web connections or that delivery services could be substantially expanded or even subsidized. Additional planning and resources spent early in the pandemic to facilitate shifts and transitions might already have been paying big dividends by late summer. But we would have needed to accept, back in March 2020, that the effects of lasting pandemic were not likely to involve a bad few months and quick snap-back to the period before the pandemic, but instead would involve lasting changes for the medium-term or even the long-term as we learned how to live with the pandemic for a sustained time.




Leave your comments
Post comment as a guest