A bubble is an economic cycle characterized by the rapid escalation of asset prices followed by a contraction. It is created by a surge in asset prices unwarranted by the fundamentals of the asset and driven by exuberant market behavior. When no more investors are willing to buy at the elevated price, a massive sell-off occurs, causing the bubble to deflate.
The pattern of a bubble is pretty consistent, despite variations in how the cycle is interpreted.
- Displacement: This stage takes place when investors start to notice a new paradigm, like a new product or technology, or historically low interest rates — basically anything that gets their attention.
- Boom: Prices start to rise at first, then get momentum as more investors enter the market. This sets up the stage for the boom. There is an overall sense of failing to jump in, causing even more people to start buying assets.
- Euphoria: When euphoria hits and asset prices skyrocket, caution is thrown out the window.
- Profit taking: Figuring out when the bubble will burst isn’t easy; once a bubble has burst, it will not inflate again. But anyone who looks at the warning signs will make money by selling off positions.
- Panic: Asset prices change course and drop as quickly as they rose. Investors and others want to liquidate them at any price. Asset prices decline as supply outshines demand.
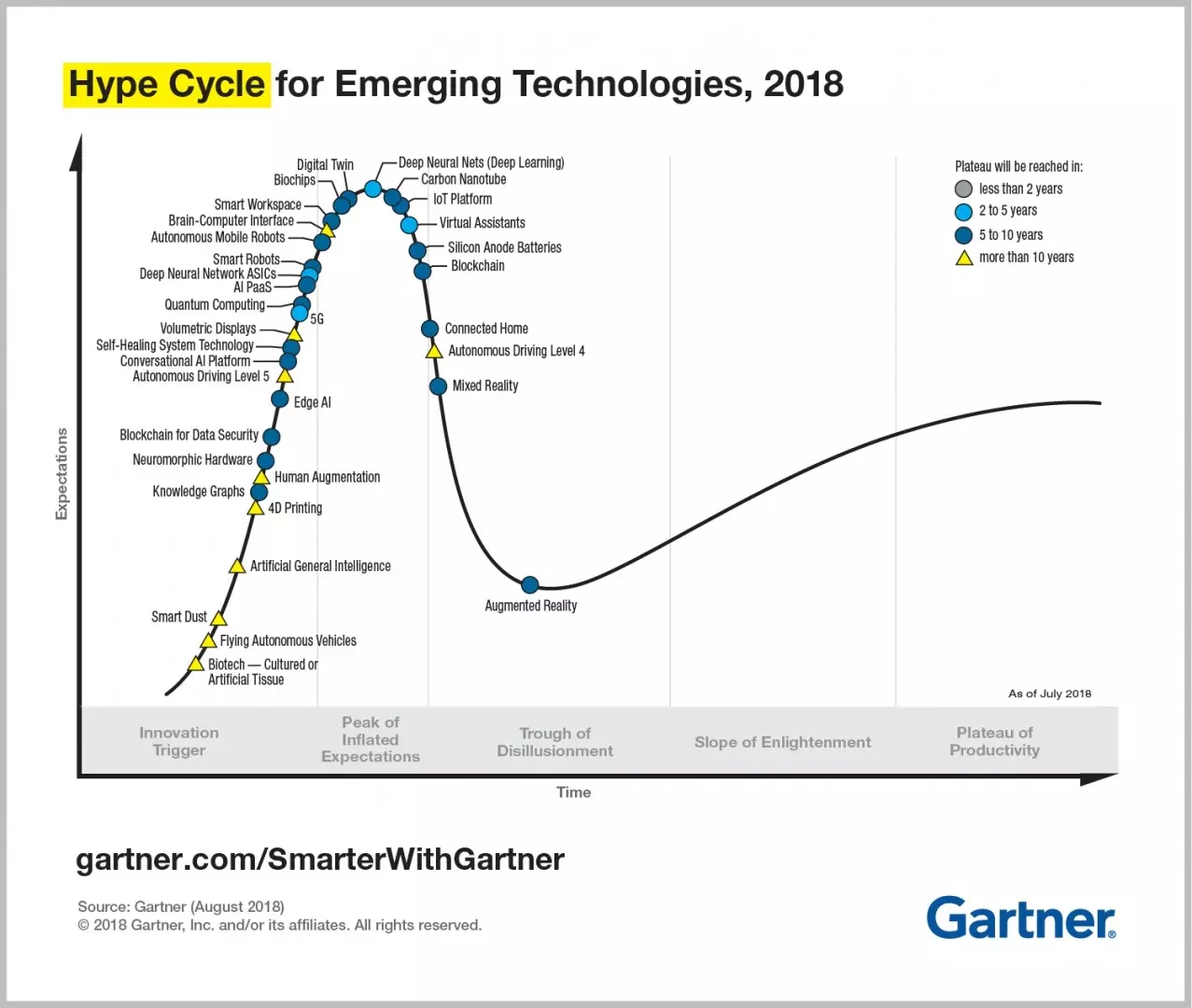
A somewhat similar model is the Gartner hype cycle:
Some think that there is a digital health bubble, an innovation bubble, a higher ed bubble , a graduate school bubble, a law school bubble and maybe even a medical school bubble.
One report suggests that leading digital health companies have not yet demonstrated substantial impact on disease burden or cost in the US health care system. The findings indicate the importance of fostering an environment, with regard to policy and the consumer market, that encourages the development of evidence-based, high-impact products.
Sick care innovation centers aren't much better.
I believe whether you believe there is a bubble or not depends on the lens you use to see progress and how you define and measure the outcome and impact of new things or new ways of doing old things:
- There might be technology bubbles, but technologies are not necessarily innovations i.e new things or old things done in a new way that create significant multiples of user defined value i.e quality/cost or ROI. The blockchain bubble is the latest example.
Here is what you should know about innovation and how to measure it.
- Sick care innovation takes a long time and constantly evolves, building on scientific and technological inventions and discoveries requiring a supportive culture, leaderpreneurs and ecosystems.
- There are significant barriers to sick care innovation dissemination and implementation, so you need to take the long view.
- Occaisionally, significant innovations, like anesthesia, antibiotics or clean water, significantly shifts the curve with a rare demonstration of a paroxysm of progress.
- There are many stakeholders in sick care and each one values a product or service differently and asks for a different value proposition. For example, doctors value quality, patients value experience and convenience. What is a bubble to one is a boon to another.
- Sick care is a highly regulated industry so the path of progress depends as much on socioeconomic and political winds as it does discovery or inventions.
- Translating inventions to innovations is the work of entrepreneurs. The sick care entrepreneurial workforce and entrepreneurial cultures are in their infancy. The entrepreneurial mindset is foreign to most sick care professionals.
- The educational and workforce models and the resulting talent pipelines producing knowledge technicians are archaic and outdated.
- The business model of Sickcare USA is not designed to create or value innovation or teach participants how to create it.
- There is no Moore's Law in sick care so innovations many times translate into increased costs, not lower ones.
There might be technological bubbles, like the dot come bust or digital health froth, but I don't think there are sick care innovation bubbles. If anything, we are just beginning to learn how to translate inventions to innovations and data to value. Given the pace of progress, many of us won't be around to see the results, let alone hear the pop.
Like the old Chinese proverb goes, "If you want to know what water is, don't ask the fish".
Arlen Meyers, MD, MBA is the President and CEO of the Society of Physician Entrepreneurs and co-editor of Digital Health Entrepreneurship.



Leave your comments
Post comment as a guest