The Journal of the American Medical Association, or JAMA as it is known to most, is among the most widely read and cited, most influential, and most prestigious medical journals in the world. The journal just called “JAMA” is the flagship, but the other vessels in the fleet, such as JAMA Internal Medicine, and JAMA Pediatrics, along with 11 others representing diverse medical specialties- are all highly respected in their own right.
Accordingly, when JAMA takes stock at year’s end, in a now recurring tradition, of what its large and global readership of physicians, other health professionals, biomedical researchers, and health journalists read, shared, and cited most- it is a robust indication of the medical community’s extant interests. Admittedly, this is only a proxy for a formal study of the medical preoccupations of the current moment, but for purposes of this column- a proxy will nicely suffice.
Here are titles for the top 5 most viewed papers of the year, in order: Push-up Capacity and Future Cardiovascular Events in Active Men; Anticholinergic Drug Exposure and the Risk of Dementia; Physical Activity Guidelines for Americans; Fluoride Exposure During Pregnancy and IQ in Offspring; Guidelines for Perioperative Care in Cardiac Surgery.
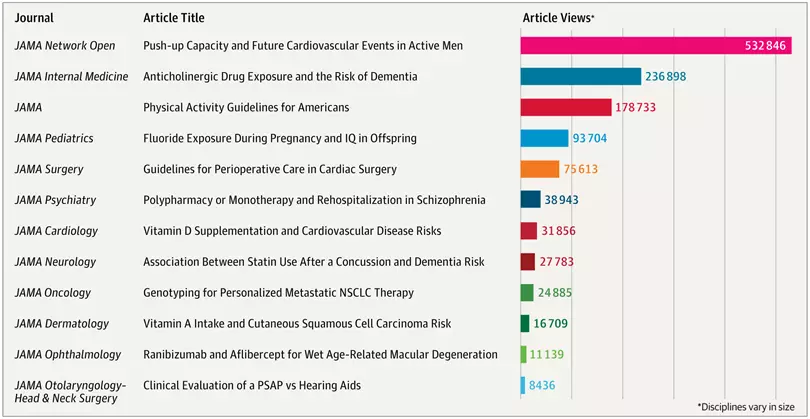
JAMA's 2019 Most-Read List
Listing these in order of popularity doesn’t quite do them full justice. The first entry was viewed on line nearly 533,000 times. The second-most-read paper was viewed fewer than half as many times; the third, fewer than 200,000 times; and the fourth, fewer than 100,000 times. The numbers drop fairly precipitously after that, impressive though they may be.\
I don’t think I can improve on this assessment by JAMA’s editorial staff: “Reflecting the remarkable interest in lifestyle medicine, our top-viewed article of the year wasn’t about a blockbuster drug but rather the humble push-up.”
Amen.
We can, however, constructively reflect further. Of the top 5 articles, only one has anything directly to do with a drug, but not because of blockbuster treatment effects. Rather, the second most popular article of JAMA’s year found a heightened risk of dementia among those exposed routinely to the large family of drugs known as anticholinergics, used to treat allergies, depression, and various disorders of the GI tract and bladder. The one drug to rank among “most popular,” in other words, was an entire class of drugs registering as a precautionary tale.
The number 3 entry, addressing physical activity guidelines, is once again a decisive entry in the lifestyle medicine category. Number 4, examining the association of fluoride exposure in drinking water during pregnancy with IQ in offspring is arguably again about lifestyle, if somewhat at the fringe. Only the last entry, presenting perioperative care guidelines, was reliably ensconced within the bounds of conventional medical practice and preoccupation- yet even here, the guidelines extended into nutritional management.
A summary judgment seems justified: the medical community- as represented by the readership of JAMA- was more provoked, intrigued, and attracted by matters of lifestyle in 2019 than by new drugs, new devices, new techniques, or specific study methods. Nothing on the list of most-read papers has any hope of garnering a Nobel Prize, while all relate to using what we know to add years to lives, and life to years.
As a health journalist, I am natively inclined to ask: “why?” about these results. As a former President of the American College of Lifestyle Medicine, I am equally inclined to infer a range of plausible answers.
First, when views of medical articles run into the many hundreds of thousands, many of those views are apt to be by lay readers along with health professionals. That does nothing to blunt the apparent interest of medical professionals in lifestyle generally and push-ups specifically; it simply attests to the breadth of that interest. Few non-medical people will feel obligated to read about the next, new drug much like many prior drugs to treat type 2 diabetes. But everyone will be interested in knowing how something they can gauge and ostensibly manage all on their own might be used to prevent a heart attack.
Second, doctors and health professionals are people, too. That seems trite, but actually, it runs deep. Perhaps you think that health professionals read medical articles only thinking about patients, or science. Often, that’s true. But not when the paper happens to be about the surgery we are having next week, or the drug we take ourselves. We are people, too, and if the subject matter relates to us personally, it likely engages a whole ancillary array of curiosity neurons. The matter of lifestyle practices - diet and nutrients, exercise, sleep, stress, toxic exposures, social connections- is relevant not only to what medical professionals do, but also- to who they are. They…are people, just like everyone else. I imagine many colleagues pushing back from the JAMA article on their computer to see how many push-ups they could do.
Third, we hear a lot on the matter of medical burnout these days. This is for many reasons beyond the scope of this column, but the formula is partly fueled by an endless cycle of diseases we have long known how to prevent, treated with drugs long known to cause side effects, leading to prescriptions to offset the ills of other prescriptions, leading to the complications and consequences of polypharmacy, and…well, you get the idea. This is a commonplace cascade in the prevailing “disease care” system where there is not only a drug for every malady, but occasionally the invention of a new malady to justify the use of some drug. Maybe doctors are starting to say: “enough!”
Certainly that is true among the devoted ranks of lifestyle medicine. The American College has more than doubled in size annually over a sequence of recent years. The membership is optimistic, energized, and full of hope about a medical future that doesn’t just tend to established disease, but actually cultivates vitality at its origins. While membership is still comparatively limited, enthusiasm for the promise of the lifestyle medicine proposition is rightly spreading far and wide.
So here we come to the deeper meaning, and real allure, of JAMA’s popularity contest. The elements of medical advance- clarifying opportunity and peril alike- of most apparent interest to medical practitioners are mostly under your control, not theirs. You do not need years of post-graduate training to walk more, or do the occasional push-up; to eat more vegetables; or attend to any of the several great lifestyle medicine imperatives. You need some reliable guidance; the will to act; and skill commensurate with your commitments.
The environment- structural and social- matters greatly as well. The choices any of us makes are always subordinate to the choices all of us have. But still, across the expanse of actionable options, the power resides far more at your feet, your fork, your fingers- than in the board rooms of Big Pharma. How refreshing!
As 2020 burgeons, perhaps you will resolve to contemplate JAMA’s verdict that the most fascinating advances in modern medicine are much about the decisions you make, and the actions you take. Perhaps we may yet find our way to a “health care” system after all. If we do, it will be in no small part…because of you.
My best wishes to you and yours for the best of health in the New Year. Prevailing medical interest points the way.





Leave your comments
Post comment as a guest