Comments (4)
Emily Carrington
Excellent, clear and concise post.
Marco Henning
Wow, god is really smart.
Beth Eveson
Perfectly explained !
Daniel Flynn
Amazing read
One of the reasons cardiology tends to advance so rapidly compared to other medical disciplines - with very noteworthy benefits, such as marked declines in both premature death and disability related to heart disease - is because of the power of surrogate markers. Surrogate markers in medicine are generally things we can measure in the short term that tell us with at least reasonable, and sometimes excellent, fidelity about likely outcomes in the long term.
Cardiology’s cup is full to the brim with good surrogate markers: LDL cholesterol, blood pressure, and heart rate for starters. In addition, there is coronary calcification scoring; lipoprotein(a); other lipids including HDL and triglycerides; CRP and other inflammatory markers; and stress testing for functional reserve. There is even an ultrasound method for direct conversations with blood vessels to ask them, in essence, “how’s it going?” that provides a very robust indication of overall vascular health. We use this method, called endothelial function testing, in my lab, and have published many papers based on it over the years.
Those medical disciplines where surrogate markers are elusive have historically been held back as a result; cancer medicine is a good example. Oncology is advancing rapidly these days with new and powerful insights about immunology, but progress has lagged behind cardiology and endocrinology in part for want of markers that show in the short term if interventions can make cancer less likely in the long term.
Surrogate markers are powerful. When you show you can alter them meaningfully, you have good evidence you can change the outcomes that really matter-notably, vitality, and longevity.
Imagine, then, if we had a surrogate marker for life expectancy itself. Imagine how powerful it would be if something we could measure that changed rapidly in response to influences and stimuli, both good and bad, reliably predicted the length of healthy life. That would be quite a boon, since otherwise, the only way to show changes in the length of life would require waiting lifetimes. I suspect we can all agree it would be something of an anti-climax to learn only on your hundredth birthday that you were likely to live to 100.
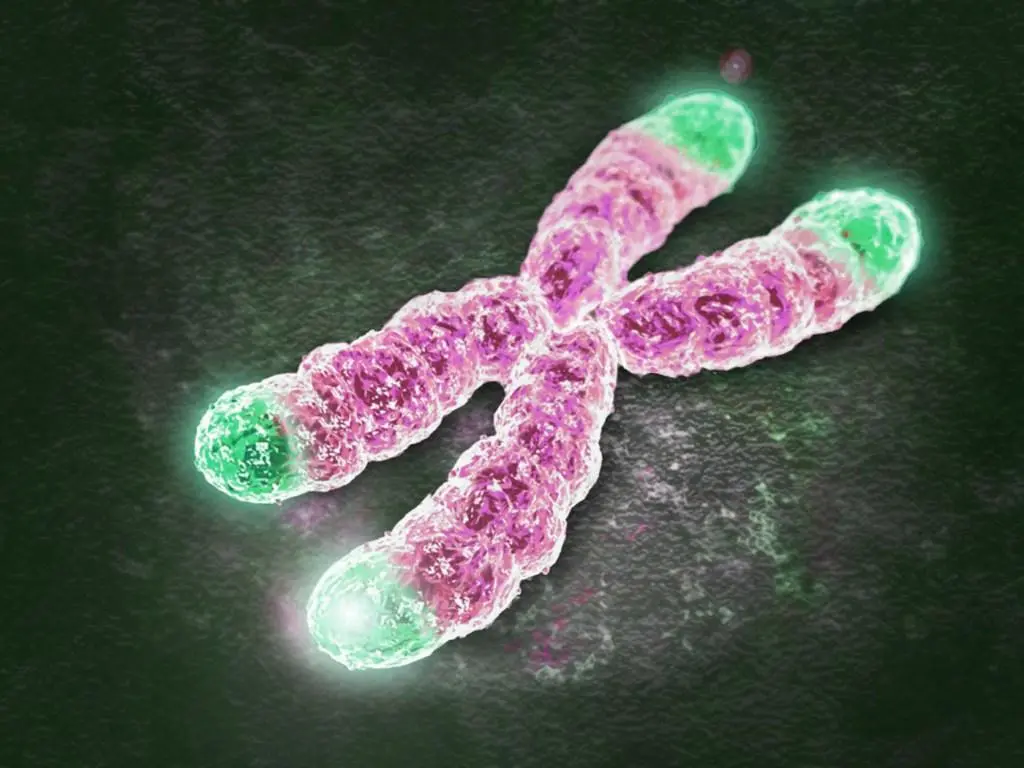
It turns out, there is just such a surrogate marker for the length of healthy life. Telomeres are, structurally, caps at the ends of our chromosomes- they have been compared to the plastic caps at the ends of shoelaces. Health-promoting exposures, or alternatively the slings and arrows of outrageous fortune, can lengthen or shorten telomeres, respectively. The length of telomeres, in turn, predicts the length of healthy life.
Not perfectly, of course; even with gloriously long telomeres, it would be imprudent to stand in the path of a moving train. But powerfully. Telomeres are among the more potent of known predictors of healthy life span, other things (like standing clear of trains) being equal. And, in fact, they are not just markers of health span, but actual mechanisms of it; vital telomeres transmit that vitality to the cells in which they reside. Imagine, then, how great it would be if we could talk directly to our telomeres, and find out how they’re doing.
Now, we can. Hold that thought for just a moment and I’ll get back to it.
First, I want to differentiate the value of surrogate markers from what we might call “duplicative markers.” Just because we can measure something doesn’t mean there is always much value in doing so.
There is a famous expression that those who have a hammer tend to see nails, and the related idea that invention can be the mother of necessity. We tend to want to use whatever tools we happen to have.
In medicine, that at times means reliance on technology to tell us what we already know. Consider, for instance, the burgeoning array of studies using some cutting edge technology, like fMRI, to study brain responses to food.
You already know that when you eat, say, French fries, you experience intense but probably rather fleeting pleasure. You also know the various feelings that come after, from hunger to guilt. What, then, does a study showing that the pleasure center in your brain lights up when you eat those fries really teach us that we didn’t already know? It’s a bit like using high-tech thermal cameras to show that warm clothes keep you warm when you’re out in the cold.
Do we really need cutting edge technology to show us changes in metabolic activity in the pleasure center of our brain to tell us we found something…pleasurable? Of course, other benefits may ensue from such research, but I do think it’s worth noting that not every difference we can measure really makes much difference to what we know. Duplicative markers in medicine abound, and to me they often seem an excuse to spend a lot of money to corroborate what we already knew for free.
Surrogate markers are different, because they tell us something we otherwise couldn’t know unless we waited for the outcomes they predict, and then - it would be too late. It’s not helpful to find out after a heart attack that we are at risk for heart disease. It’s even less helpful to find out after we die that our life expectancy isn’t everything we might wish.
Which brings us back to telomeres. Their length is predictive of the length of healthy life, while providing the lead-time necessary to do something about it. If telomeres could talk, and tell us what makes them lengthen or shrink, what makes them happy or unhappy, they would provide us compelling, powerful, actionable intelligence and a measure of control over our longevity. Conversing with telomeres would be the next best thing to sipping from the fountain of youth.
And, as noted, we all have that opportunity now. In a newly released book called The Telomere Effect, two leading experts, one of them a Nobel Prize winner, go carefully through the science enumerating the effects of diverse exposures on telomere length. Drs. Elizabeth Blackburn and Elissa Epel proceed study by study, and cover everything from stress to diet, exercise to sleep, the influences of environment when we are just in the womb to those of social interactions throughout life. They then translate each cluster of studies into practical tips you can apply.
Of course, the lifestyle prescription that’s good for our telomeres is one we already knew was good for us in general. But a vivid view of aging itself at the cellular level that does not require years and decades to elapse is a rarefied vista indeed, a truly unique window of opportunity. This book opens that window to us all.
If only telomeres could talk to us, they would provide unique insights into human aging, with the time to do something about it. It turns out they can, in the authoritative voices of Drs. Blackburn and Epel, on the pages of The Telomere Effect. Telomeres are talking now; I think everyone should listen.
Excellent, clear and concise post.
Wow, god is really smart.
Perfectly explained !
Amazing read
David L. Katz, MD, MPH, FACPM, FACP, FACLM, is the Founding Director (1998) of Yale University’s Yale-Griffin Prevention Research Center, and former President of the American College of Lifestyle Medicine. He has published roughly 200 scientific articles and textbook chapters, and 15 books to date, including multiple editions of leading textbooks in both preventive medicine, and nutrition. He has made important contributions in the areas of lifestyle interventions for health promotion; nutrient profiling; behavior modification; holistic care; and evidence-based medicine. David earned his BA degree from Dartmouth College (1984); his MD from the Albert Einstein College of Medicine (1988); and his MPH from the Yale University School of Public Health (1993). He completed sequential residency training in Internal Medicine, and Preventive Medicine/Public Health. He is a two-time diplomate of the American Board of Internal Medicine, and a board-certified specialist in Preventive Medicine/Public Health. He has received two Honorary Doctorates.
Leave your comments
Post comment as a guest